Hip Replacement Surgery - One Man's Journey. Week One
Anyone who knows me or reads this blog will know that my husband (Mr P) has suffered from arthritis in his hip for many years. He put off having surgery as his GP recommended waiting until he really needed it. This he did, but last April he'd had enough and was put on the waiting list to see a consultant. Waiting list and patient. Too words that fit together perfectly.
I'm a retired theatre sister so I know what the surgery entails but have no idea of the recovery. I googled it and everything was averages. Three to five days in hospital. Six weeks before you can drive. Six months before fully recovered. But what do these mean? How much pain is there? When will he be able to walk? What does recovered actually mean? So many questions and no real answers. I thought I would document his journey here, this is just one man's journey through hip replacement surgery in Wales. It may be different where you are, your journey may be totally different too, but I hope this gives an insight into the whole recovery process.
The Waiting List
It's called a waiting list for a very good reason, wait, wait, wait. Mr P waited too long. He was already disabled by his hip, we had stopped walking in the hills, walking anywhere really. He couldn't play with Bear because of the pain. We were just in limbo. We didn't book any holidays just incase an appointment came through. Our lives went on hold, just each day filled with more immobility and pain.Eventually he was given a consultant appointment for October. At the appointment we were told that he would go on the waiting list for surgery. The surgery would take place either before Christmas or early January. Neither happened. The ward had an outbreak of a bug and many operations were cancelled. Eventually he was given an appointment for pre-assessment in March.
Information day and Pre-Assessment Appointment
Mr P had already been to an information day telling him all about hip surgery. What to expect, what they would do. In South Wales the surgery is done under a spinal anaesthetic. This means an injection into the spine which paralyses and numbs the legs. No pain will be felt. He was also asked to measure the height of the toilet, bed and chairs so the physiotherapists could arrange any adaptations in advance.
The pre-assessment involved having a swab to check for MRSA, taking bloods, checking his observations; blood pressure, pulse rate and temperature. He was interviewed by the consultant and a nurse. It was important to check that his skin was intact, free from any spots, grazes or shaving rashes. Any break in the skin could mean cancelling the surgery. Mr P was also asked about his teeth, any bad teeth or cracks would have delayed surgery too.
Pre-Surgery
At the pre-assessment Mr P was given bottles of carbohydrate rich liquid to drink prior to surgery. These give the body a boost before the necessary fasting. It is also suggested to drink plenty and eat healthily. We eat lots of vegetables anyway so this wasn't a problem for us. The worse was that he had to stop some of his painkillers 5 days and others 2 days pre-operatively. These are any that may cause bleeding, it is all decided at pre-assessment. The problem was that he was in lots of pain the last few days. I asked him to measure his pain on a scale of one to ten. With ten being the worse pain ever. He said he was always between 8 and 10. That is a lot of pain.
We also had a visit from the appliances department to raise the sofa and give us a raised toilet seat. Check your area and what they provide. We had bought an adjustable height chair but found out afterwards they loan those out too.
 |
| Mr P bought this adjustable height chair but you can borrow one from the hospital. We didn't know. |
Day of Surgery Wednesday 12th April
Mr P had to fast from midnight and just drink the carbohydrate drinks in the morning, having nothing after 6am. The exact regime depends on whether you are having morning or afternoon surgery. He was asked to check into the ward at 7am so we guessed he was morning. Like all surgery timings are very unpredictable but he was third on the list and went down to theatre at about mid day.
Due to the spinal anaesthetic Mr P had no pain whatsoever on the day of surgery. He felt and looked fantastic. He didn't get back to the ward until late afternoon so was told to stay in bed and the physiotherapists would visit the next day to show him how to get into and out of bed and how to use the zimmer frame. Surprisingly when I asked him what the worse thing was, it was't the actual surgery. It didn't hurt and he was sedated most of the time. It was when the spinal wore off. He could lift his good leg but not his operated leg.
The surgery itself was OK. The anaesthetist explained everything that would happen, and it did, exactly as she said. I had to sit on the trolley and bend while she injected into my back, then it was tested using ice. I could feel touching but had no sense of hot or cold. I was taken into theatre and given sedation. It was like dreaming, but I knew it was real. I could hear the saw and tapping. Then I woke up in recovery.
Day One - Thursday
Once the spinal had worn off Mr P had no pain unless he moved. Unlike the pain of an arthritic hip, that is relentless, post surgery it only hurt on walking, getting up and sitting down. Whilst sat in a chair or in bed he was pain free. A lot of this was down to the amazing nurses who were always on top of his pain with regular pain relief. Aswell as his pre-operative painkillers he was given Morphine. A slow release one twice a day and a quick acting one when needed in-between. It is not sensible to allow pain to get a hold. At this stage keeping in control of the pain is vital as exercise is very important.
Mr P described the pain as 5 to 7. Except when getting into or out of a chair which was "excruciating" I'm guessing that's a 10+.
Mr P was already an expert at using a zimmer frame to walk the short distance to the bathroom and back.
The worst thing......the damage done to my quadriceps. I wasn't expecting that, I couldn't move my leg.
Day Two - Good Friday
Mr P had much less pain on walking and was now using crutches. He managed to climb and descend stairs. This is one of the criteria for being allowed to go home. Another is opening his bowels (having a poo!) and an x-ray. No sign of the poo but an x-ray booked for the next day. I couldn't see him going home for a few more days, although his pain was well managed he was struggling to get up and out of a chair. His hospital bed was electric and totally adapted, we didn't have that at home. I was also worried about the journey home. If he managed to get into the car, would we be able to get him out?
Mr P's apetite was really diminished too, not surprising really. He said the food was really nice just that he was full. I noticed the lack of vegetables and fruit, just good old fashioned food such as chicken pie and mashed potatoes.
The consultant or his registrar visited each day and was happy with his progress. In fact there always seemed to be a doctor on the ward.
Day Three - Saturday
Mr P was feeling great, walking with one crutch and just waiting for an x-ray and a poo. All the painkillers, lack of eating and being immobile can cause constipation. A bomb up the backside is called for! The x-ray was fine, the enema worked so home we go.
The average length of stay in hospital post hip surgery is 3 - 5 days. We were slightly worried that because it was the Easter holidays his discharge may have been delayed, mostly due to less staff and also the pressures for empty beds isn't so great. We were lucky, the ward runs like clockwork, everything happens when and as they said. Yesterday we didn't believe he would be fit to go home, the improvement is very fast.
So 6pm on day three Mr P was on the way home.
I have no pain in my hip at all, it was gone when I woke up in recovery. I have pain but it's different. It's the wound, stitches pulling and the swollen leg. It's like a dead leg with pain. It's different, but I can't explain the difference
Day Four - Easter Sunday
The worse thing was the night. Many trips to the toilet for a wee because of all the fluid he was drinking and possibly a side effect of surgery. Also Mr P never sleeps on his back and found doing that quite uncomfortable. In hospital the bed adjusts so he could raise the head or foot easily to get comfortable.
Sleeping on my back is the worse thing. I get numb elbows and hands. The weight of the quilt presses on my toes and my heels hurt.
I put a cushion under the quilt to raise it enough to take the pressure of his feet. I did ask about a bed cradle but the hospital do not loan them out and I didn't want to buy one just for a few weeks use. The bruising on his hip has spread right down the back of his leg and his operated leg is swollen. This is all expected and normal. Compression socks (the thick white ones) have to be worn for the first six weeks. These cause very dry skin so I am massaging in some Nivea cream to moisturise.
Day Five - Easter Monday
A short walk outside the house, up the drive and along the pavement to the neighbours drive and back again. Probably 100 metres in total. Unlike indoors the ground is uneven so Mr P found it hard going. Pain is much less and bruising much worse, leg is still swollen.
Mr P is still very tired and taking lots of short naps. This is understandable as he is not sleeping well at night and we must remember it is major surgery with a significant blood loss.
I put my old slippers on and thought he'd put my hip in the wrong way. My foot was pointing inwards not straight. Then I realised it was the shape of my old slipper!
Day Six - Tuesday
Bruising is now turning yellow and fading slightly. His operated leg is still very swollen but keeping it elevated and exercise definitely reduces the swelling. Body functioning as normal so all laxatives have been stopped, just eating lots of vegetables and drinking fluids. Mr P hates drinking water so orange juice and coffee are drinks of choice. His bruises are slowly changing colour and the edges have gone yellow.
 |
| Bruises from his knee to his bum |
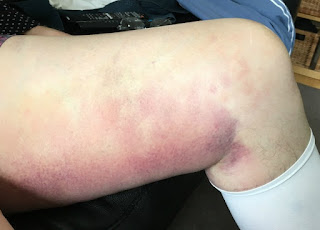 |
| The bruise is slowly turning yellow and fading |
Day Seven - Wednesday
It's been a whole week. We are into a new regime of exercising and napping. I have asked for a repeat prescription of the Morphine as it would run out before the week-end. Mr P is hoping to cut down to just one a day, one before bed, in a few days time. His pain is really well managed but he won't know if he can manage without unless he tries it. At the moment he is on morphine, paracetamol and anti-inflammatories.Morphine gives a feeling of warm drowsiness. I get little moments of absolute tiredness where I have to shut my eyes....
 |
| Mr P bought these and used them lots before surgery. Left; A Soxon. It's superb at helping to put socks on Right; A helping hand. Like a litter picker, great for picking stuff up from the floor |
 |
| This seat just sits over the toilet. It's really light and the height is adjustable. |
 |
| Our health authority provided and fitted these to raise our sofa the maximum six inches |
Tips For Before and After Hip Replacement Surgery
- Eat well leading up to the operation, if you do not have a good diet then think about taking supplementary vitamins.
- Get fit while you are waiting for your operation, have your teeth checked and fixed at the dentist. If you have any broken skin and can't heal it yourself visit your GP for advice.
- Make sure your bed and chairs are high enough to prevent you bending and to keep your hip at 90 degrees or more. Ask what aids you can borrow to raise your chairs and toilet seat.
- Buy aids that will help before and after the operation. Mr P has a "soxon" to help him put his socks on (of course with a name like that) and a grabber to stop him bending down to pick things up from the floor
- If you have railings on both sides of your stairs ask the physio for two sets of crutches, keep one upstairs and one set down stairs.
- Do not skimp on pain relief. Getting mobile is the aim and pain will stop you trying.
- Drink lots of fluids. It helps with swelling and replacing what you lost.
- If you have reduced mobility think about applying for a blue card. Mr P got one. He couldn't walk far but worse he couldn't get in or out of the car. Disabled spaces give that bit extra room.
- Do the exercises. Walk around the house. Just keep moving.
- Be positive. A positive attitude really helps with recovery.
The first week is over and Mr P is doing really well. His pain is between three and five out of ten. He says its more discomfort caused by the swelling than actual pain. His new hip is fantastic and I am already thinking about the walks we can do together again.
Follow me on
Bloglovin | Facebook | Twitter
Bloglovin | Facebook | Twitter


Well done Mr P. It sounds like everything is going so great. It sounds and looks like all the aids and adaptions are a great help. I hope he continues to make a good recovery x
ReplyDeleteThank you. He's doing great. I am so impressed with his determination for it to work. He is exercising and walking around the house. It's amazing what he can do just one week later xx
DeleteMy Father-in-law is three months on from surgery. He has done particularly well because he did absolutely all the walking he was asked to do - which was a lot. Two walks per day - initially very short. He was so diligent. He had knee pain but that was because for the first time in ages he is standing up straight and his knees were not used to that. Best wishes for the rest of the recovery. BTW Ikea sell very cheap long-handled shoe horns, which are so useful!
ReplyDeleteThank you so much for this! We have a shoe horn from there, it looks like a snake and my grandson always says ssssss when he sees it.
DeleteMy husband is being diligent too, he's doing everything exactly as he's been told. His leg is very swollen and that is what is causing him pain. If he can get the swelling down he would be almost free of pain.
This comment has been removed by the author.
ReplyDelete